eOrganic author:
Linda Tikofsky
Source:
Adapted with permission from: Mendenhall, K. (ed.) 2009. The organic dairy handbook: a comprehensive guide for the transition and beyond. Northeast Organic Farming Asociation of New York, Inc., Cobleskill, NY. (Available online at: http://www.nofany.org/organic-farming/technical-assistance/organic-dairy, verified 18 July 2012).
Introduction: Defining Milk Quality
Milk quality can mean many things to many people. Consumers expect that their milk will have a consistent appearance, pleasant taste, and last a week or more in their refrigerator. According to the Pasteurized Milk Ordinance (PMO), Grade A milk has a Somatic Cell Count (SCC) of less than 750,000 cells/ml and a standard plate count (SPC) of less than 100,000 colony-forming-units (cfu)/ml and is free of added water and harmful residues above a designated tolerance limit. These are the minimum standards. Organic processors are willing to pay for high quality so there is opportunity for dairy producers to increase their milk check substantially by focusing on udder health and limiting mastitis on their farms. Many processors are reluctant to receive milk that is consistently greater than 400,000 cells/ml.
Somatic Cell Counts (SCC)
In a healthy udder, somatic cells are epithelial cells from the lining of the mammary gland and some types of white blood cells. A healthy gland should have cell counts less than 100,000 cells/ml and typically, counts are much lower than that (less than 25,000 cells/ml).
When bacteria invade the gland, the few white blood cells normally present send out an alarm to the rest of the body and recruit thousands of additional white blood cells from the blood stream to come into the mammary gland to fight infection. Infected glands have SCCs greater than 250,000 cells/ml and often the counts reach into the millions. If all goes well, these white blood cells kill the invading bacteria and the SCC of the gland decrease to less than 100,000 cells/ml within 30 days. We can estimate the number of infected quarters in a herd and the impact on production from the bulk milk SCC (see Table 1).
| Bulk Tank SCC | Percent infected quarters in herd | Percent production loss |
| 200,000 | 6 | 0 |
| 500,000 | 16 | 6 |
| 750,000 | 25 | 12 |
| 1,000,000 | 32 | 18 |
| 1,500,000 | 48 | 29 |
| Source: Britt, J. 1987. Herd linear scores versus bulk tank sampling. Proceedings of National Mastitis Council Annual Meeting. Orlando, FL. | ||
Regularly monitoring SCC at both the herd and individual animal levels provides you with valuable information to help manage milk quality and improve profitability. Monitoring will help you detect new infections so that appropriate therapies can be administered early in the course of the disease. Monitoring chronically infected cows will help you identify those for culling, early dry off, or candidates for potential nurse cows. You can also follow SCCs after administering therapies to determine whether the treatment was successful. There are many ways to monitor SCC on farms and they vary in terms of cost, ease of use, and reliability of information (see Table 2).
| Cell Counting Option | Cost | Accuracy | Limitations |
| Monthly DHIA testing | $0.80 to $1.50 per cow per month | Excellent | • Only gives SCC for the cow for that single day • SCC can fluctuate day to day |
| Cow-side direct cell counting | • $300 to 3,000 for initial unit • $1.50 per cow per test | Very good to adequate | • More expensive devices have better accuracy |
| California or Wisconsin Mastitis Test (CMT/WMT) | • A few cents per test | Fair | • More accurate for very high cell counts • Can be difficult to read for SCC< 1,000,000 cells/ml |
| Electrical conductivity | • Hand-held unit: $300–400 • In-line monitor: thousands | Highly variable | • Best used for early detection of clinical mastitis • Reliability for chronic or subclinical mastitis is limited |
Bacteria Counts
Several factors affect bacteria counts in raw milk: cleanliness of the cow’s teats and udder, udder infections (mastitis), cleanliness of milking machines, and milk storage and cooling. Excessive bacteria counts impact shelf life, flavor, and increase the risk of foodborne diseases (e.g., Salmonella, Listeria) in the milk supply. Pasteurization effectively kills a majority of the bacteria in milk, but it does not sterilize milk. Thus, when milk has extremely high bacteria counts, a portion of bacteria can survive the pasteurization process and be present in the final product.
Mastitis-causing bacteria may increase bacteria counts in raw milk. These are usually bacteria in the streptococcus family (Streptococcus agalactiae, Streptococcus uberis, and Streptococcus dysgalactiae) and infrequently, E. coli. The majority of bacteria issues in raw milk are related to poor cleaning or improper cooling of milk.
Dairy producers can ensure that their milk has low bacteria counts by adhering to the following practices.
- Always milk clean, dry teats.
- Keep milk from cows infected with mastitis out of the bulk tank.
- Ensure that the equipment wash chemicals are appropriate for the farm’s water hardness and that correct amounts are used.
- Check that rinse and wash water temperatures are within the recommended ranges.
- Sanitize the equipment immediately before milking.
- Cool milk to less than 45°F and preferably to 40°F.
Diseases of the Teats and External Udder
Weather and housing conditions, bedding, and infectious disease may affect the outside surface of the udder and teats. These diseases can affect milking or harbor bacteria (e.g., Staph aureus), resulting in new mastitis cases.
| Disease | Cause | Contributing Factors | Signs | Treatment or Management |
| Mammilitis | Herpes virus | Heifers, winter weather | Blisters, scabs, "wooden teats" | Chlorhexidine teat dips in winter, vaccination |
| Warts | Papilloma virus | Contagious spread at milking | Small, teat colored bump | Surgical removal, vaccination, chlorhexidine dips |
| Udder rot | Unknown | Udder edema, mange mites, udder shape | Skin infection between halves of udder or between leg and udder | Scrub with antiseptic soap (iodine or chlorhexidine), dry the area, calendula salve, raw honey |
Mastitis
Mastitis is an inflammation of the mammary gland in response to injury. Usually, this injury occurs via infection by a microorganism, most commonly bacterial, but physical and chemical trauma can also cause mastitis. If contagious mastitis is present in a herd planning to transition to organic dairy production, the farmer should make all efforts to identify, treat, and/or cull the infected animals prior to transition. In established organic herds, contagious mastitis can be more of a headache, but it can be managed with continued effort and monitoring. Alternative therapy regimens usually yield disappointing results and are often impractical for large numbers of animals. More than 100 organisms are capable of causing mastitis in cows and most of these are bacteria. These bacteria may be considered contagious (living primarily in the cow's udder and spreading at milking time) or environmental (living in bedding, manure and mud and infecting cows anytime). See Table 4.
There are two classifications of the degree of mastitis inflammation: clinical and subclinical.
- Clinical mastitis: Visible changes in milk or udder (redness, swelling, pain, clots and flakes). Most commonly caused by environmental bacteria.
- Subclinical mastitis: No physical changes in udder or milk, but large increases in microscopic cells and bacteria. You can detect subclinical mastitis with one of the cell counting options mentioned previously or by culturing a milk sample. Contagious mastitis commonly causes subclinical mastitis. For every one case of clinical mastitis in a herd, there may be 15 to 40 cases of subclinical mastitis.
| Contagious Mastitis | Organism | Common Sources | Transmission | Symptoms and Impacts on Milk Quality | Best Management Practices |
| Streptococcus agalactiae “Strep ag” | • Infected udders | • Cow to cow at milking time: on inflations and hands | • Very high somatic cells counts • Decreased milk production • High bacteria counts | 1. Identify infected cows through whole herd milk culture 2. Milk infected cows last 3. Cull high SCC cows (cull ALL Myco. cows) 4. Wear gloves to milk 5. Post dip 6. Control flies 7. Culture herd replacements | |
| Staphylococcus aureus “Staph aureus” | • Infected udders • Skin | • Similar to Strep ag • Biting flies • Cross-suckling by calves | • Fluctuating somatic cell counts • Occasionally, clinical mastitis • Scarring of udder • May cause gangren | ||
| Mycoplasma species | • Infected udders • Cows and heifers with respiratory disease | • Similar to Strep ag and Staph aureus • Coughing and sneezing • Calves may be infected by drinking infected milk | • High SCC • Decreased milk production in one or more quarters • Swollen joints • Coughing and pneumonia • Calves may have head tilt or ear infectio | ||
| Corynebacterium bovis (C. bovis) | • Teat skin | • Cow to cow at milking | • Occasional clinical mastitis • Minimal increase of SCC | 1. Post dip with iodine-based teat dip 2. Apply teat dip with a cup | |
| Environmental Mastitis | Environmental streptococci (Strep uberis & Strep dysgalactiae) | • Bedding, manure, and soil | • Between milkings from environment • At dry off and during prefresh period | • High SCC and sometimes high bacteria counts • Clinical mastitis | 1. Clean cows 2. Clean environment 3. Well-bedded stalls 4. Good premilking teat preparation 5. Well-maintained milking equipment 6. Clean dip cups regularly 7. Good fly control 8. Fence ponds and standing water in pastures 9. Rotate pastures to avoid mudholes from developing under trees 10. Store bedding properly to avoid contamination and moisture 11. Coliform vaccination for herds with E. coli and Klebsiella problems. |
| Environmental staphylococci (Coagulase negative staph—CNS) | • Bedding, manure, and soil | • Between milkings from environment | • Mild increase in SCC | ||
| Escherichia coli (E. coli) | • Manure | • Between milkings from environment • More common in summer | • Acute mastitis: watery milk, hot hard quarter, very sick cow, may cause death | ||
| Klebsiella species | • Manure, soil | • Between milkings from environment • More common in summer | • Acute mastitis: watery milk, hot hard quarter, very sick cow, may cause death • Cows that survive will usually have chronic quarters | ||
| Pseudomonas species | • Contaminated water or hoses | • Between milkings • At milking time from water • From contaminated mastitis tubes | • Severe, chronic mastitis | ||
| Serratia species | • Contaminated teat dip • Contaminated water | • Between milkings from environment • At milking time from contaminated dip cups | • Chronic mastitis | ||
| Arcanobacterium pyogenes “summer mastitis” | • Soil, dry cow and heifer environments • Biting flies | • During dry period • After teat injury | • Thick, smelly discharge from swollen quarter | ||
| Prototheca species (algae mastitis) | • Mud, silage juice, pasture, manure | • Between milkings from environment | • Chronic mastitis • Cows can shed in their manure |
Mastitis Management
Management of mastitis in a herd should focus on preventing new infections rather than treating infections as they occur. Even in conventional herds where antibiotic treatment is allowed, identifying the risks for new infections and adopting best management to reduce those risks is the key to producing high-quality milk and increasing the profitability of the farm.
Mastitis Basic Management Strategies
- Good milking procedures.
- Udder wash/predip: Before you attach the milking units, wash or predip teats and wipe clean with single-use towels.
- Forestrip into cup or gutter: Stimulates milk letdown response and helps identify clinical mastitis early.
- Nitrile or latex gloves: Gloved hands are more easily disinfected between cows or when contaminated with milk or manure.
- Milking order: Milk cows with contagious mastitis last.
- Overmilking/machine stripping: Machine stripping damages teat ends causing cracks that are more likely to be colonized by S. aureus.
- Post-milking teat dipping: Apply immediately after milking to kill bacteria left on the teats by the inflations and to protect the teat end until it closes.
- Maintain milking equipment regularly.
- Evaluate equipment biannually: A qualified individual should evaluate the mechanical milking system at least twice a year and perform dynamic testing while the system is operating.
- Replace liners: Replace rubber milking liners every 800 cow milkings or every 60 days, whichever comes first. Rubber used longer than this deteriorates and will develop microscopic cracks and ridges that hold mastitis bacteria even through the wash cycle.
- Dry cow management.
- Organic dairy production does not allow the use of dry cow antibiotics or external/internal teat sealants. However, the dry period is an important time for udder health improvement and the rejuvenation of milking tissue.
- Reduce feed intake one week before dry off to decrease production.
- Dip teat end with teat dip twice daily for a week after dry off.
- Feed adequate amount of selenium and vitamin E in the dry period.
- Keep dry cow housing and bedding clean and dry. Hygiene is essential!
- Mastitis management.
- Figure 1 will guide treatment of mastitis through its decision tree. Healthy cows with good immune systems will often recover with no-to-minimal treatment. Cows with severe acute mastitis require measures to support their immune systems, allowing the opportunity for natural healing.
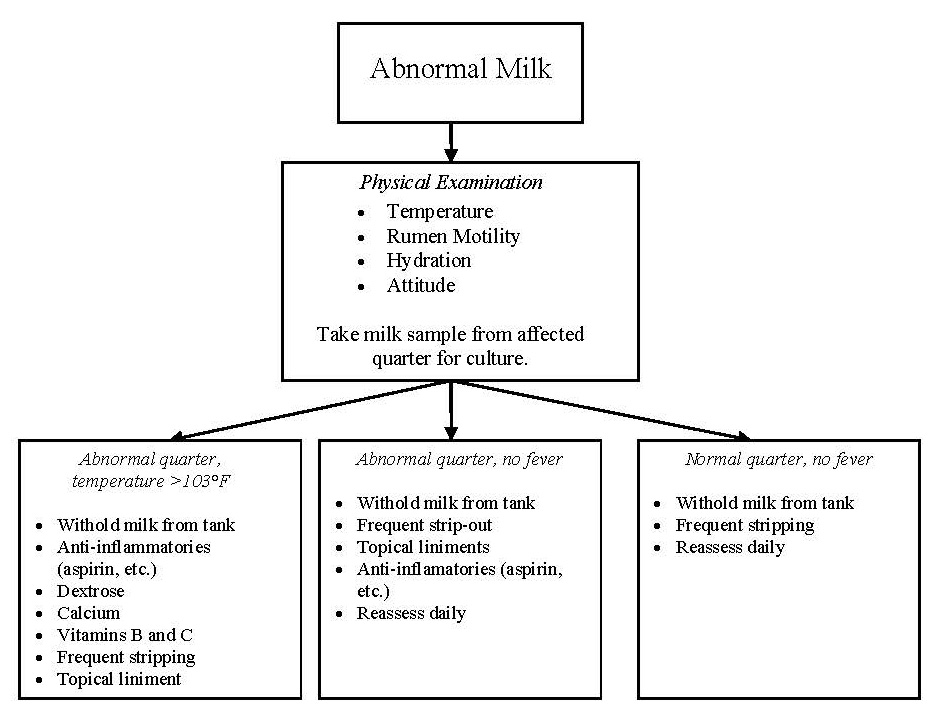
Figure 1. Mastitis treatment decision tree.
For specific mastitis treatments, dosages, and additional information, consult with your herd veterinarian or one of the resources listed at the end of this article. When administering medications, administer intramammary infusions with great care so as not to introduce new bacteria into the mammary gland with the medication. Medications should be sterile and packaged in single-use infusion tubes. Proper procures are to dip and wipe the teat, then clean the teat end with cotton moistened with rubbing alcohol, and lastly infuse the quarter. After infusion, dip the teat again.
Remember that all the milk house cleaners, sanitizers and teat dips must be listed in the OSP so they can be reviewed and approved by the certifier prior to use.
Also in This Series
This article is part of a series discussing organic dairy herd health. For more information, see the following articles.
- Organic Dairy Herd Health: General Concepts
- Alternative and Complementary Treatment and Medicines
- Youngstock Management
- Effect of Housing and Cow Comfort on Health and Disease
- Reproductive Management from Breeding through Freshening
- Hoof Health and Lameness
- External and Internal Pests and Parasites
- Managing Disease in the Organic Herd
References and Citations
- Animal Welfare Information Center Bulletin [Online]. USDA National Agricultural Library. Available at: http://awic.nal.usda.gov/publications/animal-welfare-information-center-bulletin (verified 15 June 2012).
- Britt, J. 1987. Herd linear scores versus bulk tank sampling. Proceedings of National Mastitis Council Annual Meeting. Orlando, FL.
- de Bairacli Levy, J. 1991. The complete herbal handbook for farm and stable. Faber and Faber, London.
- Dettloff, P. 2004. Alternative treatments for ruminant animals. Acres U.S.A., Austin, TX
- Fraser, A. F. 1997. Farm Animal Behaviour and Welfare. CABI Publishing, New York, NY.
- Grandin, T. 2011. Outline of cow welfare critical control points for dairies [Online]. Grandin Livestock Handling Systems, Fort Collins, CO. Available at: http://www.grandin.com/cow.welfare.ccp.html (verified 15 June 2012).
- Karreman, H. 2006. Treating dairy cows naturally: Thoughts and strategies. Acres U.S.A., Austin, TX.
- Macleod, G. 2004. A veterinary materia medica and clinical repertory: With materia medica of the nosodes. Random House: UK.
- New York State Cattle Health Assurance Program Welfare/Cattle Care Module [Online]. New York State Cattle Health Assurance Program. Available at: http://www.nyschap.vet.cornell.edu/module/welfare/welfare.asp (Verified 15 June 2012).
- Sheaffer, C.Er. 2003. Homeopathy for the herd: A farmers guide to low-cost, non-toxic veterinary care for cattle. Acres U.S.A., Austin, TX.
- U.S. Food and Drug Administration. 2009. Grade "A" pasteurized milk ordinance. U.S. Department of Health and Human Services, Public Health Service, Food and Drug Administration. (Available online at: http://www.fda.gov/downloads/Food/FoodSafety/Product-SpecificInformation/MilkSafety/NationalConferenceonInterstateMilkShipmentsNCIMSModelDocuments/UCM209789.pdf) (verified 15 June 2012).
- United States Department of Agriculture. 2000. National organic program: Final rule. Codified at 7 C.F.R., part 205. (Available online at: http://www.ecfr.gov/cgi-bin/retrieveECFR?gp=1&SID=f8b2967603d1a188e3b2b1ce9afbee3c&ty=HTML&h=L&n=7y3.1.1.9.32&r=PART) (verified 7 Feb 2013).
- Verkade, T. 2001. Homeopathic handbook for dairy farming. Homepathic Farm Support Ltd., Hamilton 3240, New Zealand.
- Whole Foods Market Animal Welfare [Online]. Whole Foods Market. Available at: http://www.wholefoodsmarket.com/meat/welfare.php (verified 15 June 2012).
- Wynn, S. and B. Fougere. 2007. Veterinary herbal medicine. Mosby-Elvesier, St. Louis, MO.



